Laser-based processing of a novel near-beta Ti-Nb-Zr alloy for the production and functionalization of bone implants for patients with age-related osteoporosis
Project Aims
As a result of demographic change and increased life expectancy, the prevalence of age-related diseases such as osteoporosis continues to rise. This is creating a need for improved implants.
The "OsteoLas" project aims to develop a holistic laser-based process chain for the manufacturing of orthopedic implants specifically tailored to the needs of osteoporosis patients. This includes the additive manufacturing of customizable bone implants from a special titanium alloy (Ti-13Nb-13Zr) using laser powder bed fusion (LPBF). This approach enables the creation of molded implant bodies with maximum design flexibility, low stiffness and high strength.
Another focus of the project is the creation of biofunctional surface structures on these LPBF implants. This is done by targeted microstructuring using the direct laser interference patterning (DLIP) method. This technique aims to increase the biocompatibility of the implants by creating hierarchical surface structures with micro- and nanometer resolution on complex 3D geometries. This is expected to promote bone tissue accretion and improve the stability of the implant-bone connection.
Overall, the project aims to optimize the production of implants for osteoporosis patients while establishing Saxony as a leading location in innovative laser process-based implant manufacturing, both nationally and internationally. The project brings together expert groups from the Leibniz Institute for Solid State and Materials Research (IFW) Dresden and the Fraunhofer Institute for Material and Beam Technology (IWS) Dresden to create synergy effects and realize a systemic process chain for customizable implants. Possible applications and further developments in the areas of material fatigue under biomechanically relevant loading scenarios, preclinical studies and technology transfer to industrial partners are also being considered.
Results
The OsteoLas project explored the development of advanced orthopedic implants with a focus on additive manufacturing and surface modification techniques. The project consisted of multiple steps, the key findings of which are as follows:
Additive Manufacturing: The project used Laser Powder Bed Fusion (LPBF) to additively manufacture a near-beta Ti-13Nb-13Zr alloy for orthopedic implants. Researchers optimized the process parameters and post-processed the parts through heat treatment to achieve improved mechanical properties and low elastic modulus, making them suitable for load-bearing implants. The corrosion resistance of these LPBF-produced implants was comparable to traditionally manufactured alloys.
Direct Laser Interference Patterning (DLIP): DLIP was employed to create complex surface patterns on the Ti-13Nb-13Zr alloy. Using different laser wavelengths and pulse durations, various surface structures, including Laser-induced periodic surface structures (LIPSS) with different spatial frequencies and feature sizes were produced. Using nanosecond-pulsed DLIP, single-scale surface textures were obtained. Using pico- and femtosecond DLIP, hierarchical surface pattern comprised of DLIP and LIPSS could be obtained. The laser parameter space and the resulting surface pattern geometries were extensively characterized. This provided opportunities to tailor the surface properties of the implants.
Extensive surface characterization: For a preliminary selection of optimized DLIP-topographies, human bone marrow stromal cells were cultivated on different DLIP-textured LPBF-produced Ti-13Nb-13Zr samples. Their biocompatibility was qualitatively asses on the basis of fluorescence microcopy measurements.
Two DLIP textures (one single-scale and on hierarchical) with comparable depth profiles (1-2 µm depth) and a spatial period of 5 µm were selected for further characterization based on their exhibited advantageous cell attachment. Multiscale surface chemical and
microstructural analyses (AES, XPS, XRD, SEM, TEM, GD-OES, contact angle) of those DLIP states were performed for understanding the corrosion behavior in a physiological PBS solution. Increased beta-phase fractions and uniformly thick passive layers of ns-DLIP surfaces led to enhanced corrosion stability compared to ps-DLIP with defective surface oxide. Both DLIP states control the surface wettability, thereby limiting corrosion and metal ion release rates, which is beneficial for implant applications.
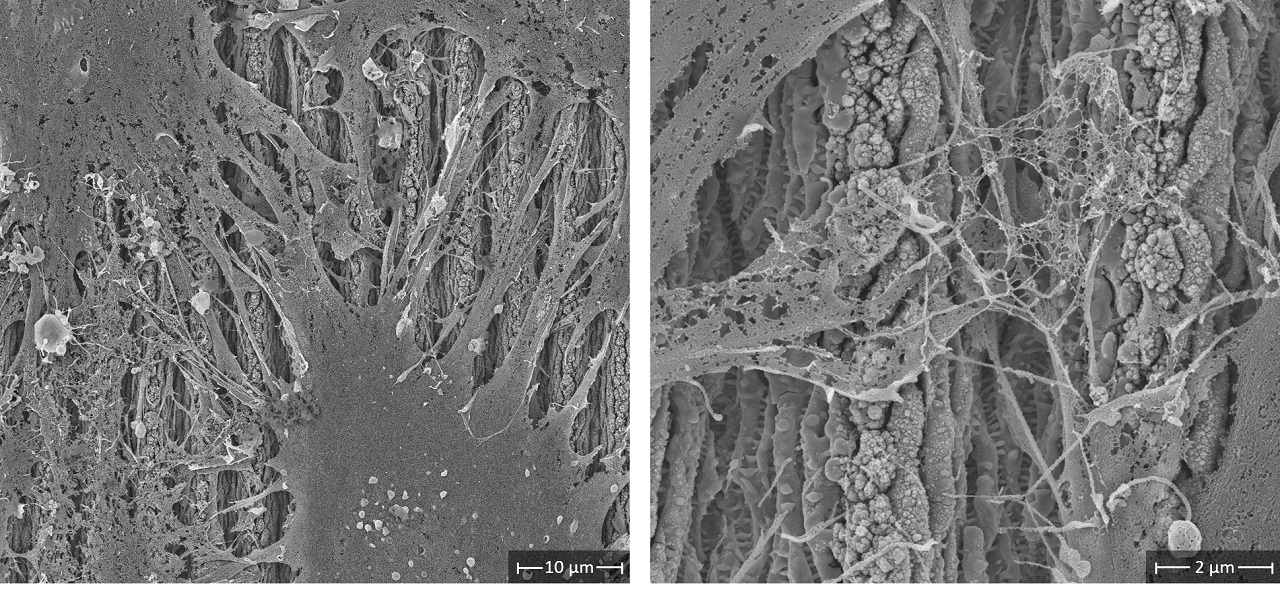
Biocompatibility Enhancement: These single-scale and multi-scale surface textures on 3D-printed titanium implants were tested with human bone marrow stromal cells using MTS and TNAP assays. The results showed that both types of textures significantly increased metabolic activity and cell proliferation compared to untextured specimens. The surface topography, roughness, and surface chemistry influenced cell behavior, including adhesion, proliferation, and differentiation.
Overall, the OsteoLas project successfully demonstrated the potential of additive manufacturing and surface modification techniques, such as DLIP, to produce biocompatible and mechanically suitable orthopedic implants. These innovations hold promise for improving patient-specific implants and enhancing osseointegration for better bone healing.
 Fraunhofer Institute for Material and Beam Technology IWS
Fraunhofer Institute for Material and Beam Technology IWS